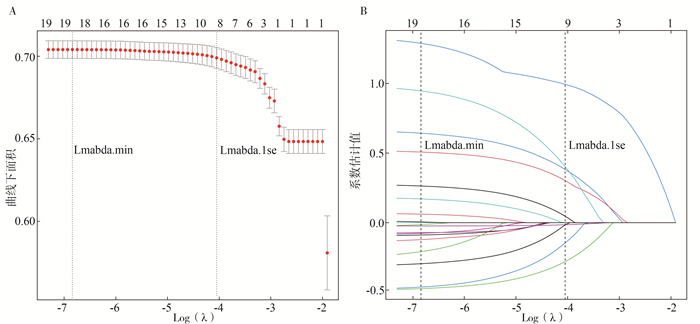
Based on Lasso-Logistic regression to build a continued drug use risk prediction model for methadone maintenance treatment patients
-
摘要:
目的 探讨美沙酮维持治疗(methadone maintenance treatment, MMT)门诊患者入组治疗后继续使用毒品的影响因素,构建并验证继续使用毒品风险预测模型。 方法 以2013―2017年入组云南省MMT门诊的患者为研究对象,利用Lasso回归筛选出与患者继续使用毒品相关的变量,用于构建多因素Logistic回归分析模型;采用Bootstrap法进行模型内部验证并用列线图实现模型的可视化。 结果 本研究纳入的7 899名研究对象在接受治疗的6个月内,共有4 125(52.22%)人发生了继续使用毒品行为。Lasso回归筛选出9个与继续使用毒品相关的变量,分别是男性、独居、目前无工作、家庭关系一般、家庭关系较差、吸毒时长、过去1个月有注射行为、过去3个月曾被公安抓捕和过去3个月因吸毒而违法犯罪。预测模型的曲线下面积(area under curve, AUC)为0.70(95% CI: 0.69~0.72)。 结论 本研究构建的风险预测模型具有较好的预测能力,可用于指导MMT门诊工作人员提早识别出治疗期间继续使用毒品的高风险人群。 Abstract:Objective To explore the associated risk factors of continued drug use in methadone maintenance treatment (MMT) patients, and to build a continued drug use risk prediction model. Methods Opioid users who newly enrolled in MMT clinics in Yunnan Province during 2013-2017 were included in the study. We used Lasso regression analysis to screen risk factors for continued drug use. We constructed a prediction model based on screened risk factors above by multivariable Logistic regression analysis. We used bootstrap method to internally validate the model. Further, a nomogram was established to visualize the model. Results Of 7 899 eligible patients, 4 125(52.22%) cases continued to drug use in the first 6 months following enrollment. Nine variables collected at baseline for MMT patients were selected for the prediction model. i.e., male, living alone, unemployed, normal family relationship, bad family relationship, duration of drug use, drug injection behavior in past month, caught by the police in past three months, and criminal behavior in past three months. The model exhibited well discrimination with an area under curve (AUC) of 0.70 (95% CI: 0.69-0.72). Conclusion The model presents good performance in predicting continued drug use risk for MMT newly enrolled patients, which can be used to help clinic staff to find early patients at high-risk of continuing use opioid while receiving MMT service. -
Key words:
- Methadone maintenance treatment /
- Lasso /
- Risk prediction model /
- Nomogram
-
表 1 MMT患者基线特征
Table 1. Baseline characteristics of MMT patients
基线特征 人数(例) 构成比(%) 性别 男 7 031 89.01 女 868 10.99 年龄(岁) <35 1 912 24.21 35~<50 4 498 56.94 ≥50 1 489 18.85 民族 汉族 5 155 65.26 非汉族 2 744 34.74 文化程度 文盲 566 7.17 小学/初中 6 415 81.21 高中及以上 918 11.62 婚姻状况 已婚有配偶 3 990 50.51 丧偶/离婚 1 244 15.75 未婚 2 665 33.74 居住状况 与家人/亲戚/朋友 6 783 85.87 独居 1 116 14.13 工作状况 有工作 2 533 32.07 无工作 5 366 67.93 家庭关系 良好 3 625 45.89 一般 2 049 25.94 较差 2 225 28.17 吸毒时长(年) <5 2 630 23.32 5~<10 1 471 28.60 10~<15 1 355 17.15 ≥15 2 443 30.93 过去1个月内和吸毒朋友交往次数 < 1次/周 405 5.13 1~ < 7次/周 5 279 66.83 ≥7次/周 2 215 28.04 入组MMT年份(年) 2013 2 421 30.65 2014 1 777 22.50 2015 1 565 19.81 2016 1 235 15.63 2017 901 11.41 表 2 多因素Logistic回归分析模型结果
Table 2. Results of multivariable Logistic regression model
变量 β值 Wald值 OR(95% CI)值 P值 性别 女性 1.00 男性 0.31 15.77 1.37(1.17~1.60) < 0.001 居住状况 非独居 1.00 独居 0.64 69.27 1.90(1.63~2.20) < 0.001 工作状况 有工作 1.00 无工作 0.49 85.80 1.63(1.47~1.80) < 0.001 家庭关系 良好 1.00 一般 0.28 22.70 1.33(1.18~1.49) < 0.001 较差 0.53 78.56 1.69(1.51~1.90) < 0.001 吸毒时长(年) < 5 1.00 5~ < 10 -0.14 3.89 0.87(0.76~1.00) 0.049 10~ < 15 -0.41 31.85 0.67(0.58~0.77) < 0.001 ≥15 -0.54 76.86 0.58(0.52~0.66) < 0.001 过去1个月有注射行为 否 1.00 是 1.12 504.85 3.08(2.79~3.40) < 0.001 过去3个月曾被公安抓捕 否 1.00 是 -0.48 25.92 0.62(0.52~0.75) < 0.001 过去3个月因吸毒而违法犯罪 否 1.00 是 0.98 30.11 2.67(1.88~3.79) < 0.001 -
[1] Sullivan SG, Wu Z, Rou K, et al. Who uses methadone services in China? Monitoring the world's largest methadone programme[J]. Addiction, 2015, 110: 29-39. DOI: 10.1111/add.12781. [2] Moradinazar M, Farnia V, Alikhani M, et al. Factors related to relapse in patients with substance-related disorders under methadone maintenance therapy: decision tree analysis[J]. Oman Med J, 2020, 35(1): e89. DOI: 10.5001/omj.2020.07. [3] Yin W, Hao Y, Sun X, et al. Scaling up the national methadone maintenance treatment program in China: achievements and challenges[J]. Int J Epidemiol, 2010, 39: ii29-ii37. DOI: 10.1093/ije/dyq210. [4] Naji L, Dennis BB, Bawor M, et al. A prospective study to investigate predictors of relapse among patients with opioid use disorder treated with methadone[J]. Subst Abuse, 2016, 10: 9-18. DOI: 10.4137/sart.s37030. [5] Kassani A, Niazi M, Hassanzadeh J, et al. Survival analysis of drug abuse relapse in addiction treatment centers[J]. Int J High Risk Behav Addict, 2015, 4(3): e23402. DOI: 10.5812/ijhrba.23402. [6] Clark RE, Baxter JD, Aweh G, et al. Risk factors for relapse and higher costs among Medicaid members with opioid dependence or abuse: opioid agonists, comorbidities, and treatment history[J]. J Subst Abuse Treat, 2015, 57: 75-80. DOI: 10.1016/j.jsat.2015.05.001. [7] Sullivan SG, Wu Z, Cao X, et al. Continued drug use during methadone treatment in China: a retrospective analysis of 19, 026 service users[J]. J Subst Abuse Treat, 2014, 47(1): 86-92. DOI: 10.1016/j.jsat.2013.12.004. [8] Kelly JF, Hoeppner BB, Urbanoski KA, et al. Predicting relapse among young adults: psychometric validation of the Advanced WArning of RElapse (AWARE) scale[J]. Addict Behav, 2011, 36(10): 987-993. DOI: 10.1016/j.addbeh.2011.05.013. [9] Andersson HW, Wenaas M, Nordfj rn T. Relapse after inpatient substance use treatment: a prospective cohort study among users of illicit substances[J]. Addict Behav, 2019, 90: 222-228. DOI: 10.1016/j.addbeh.2018.11.008. [10] Flórez-Salamanca L, Secades-Villa R, Budney AJ, et al. Probability and predictors of cannabis use disorders relapse: results of the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC)[J]. Drug Alcohol Depend, 2013, 132(1-2): 127-133. DOI: 10.1016/j.drugalcdep.2013.01.013. [11] Weinberger AH, Platt J, Esan H, et al. Cigarette smoking is associated with increased risk of substance use disorder relapse: a nationally representative, prospective longitudinal investigation[J]. J Clin Psychiatry, 2017, 78(2): e152-e160. DOI: 10.4088/JCP.15m10062. [12] Mohammadpoorasl A, Fakhari A, Akbari H, et al. Addiction relapse and its predictors: a prospective study[J]. J Addict Res Ther, 2012, 3(1): 1-3. DOI: 10.4172/2155-6105.1000122. [13] Shah NG, Galai N, Celentano DD, et al. Longitudinal predictors of injection cessation and subsequent relapse among a cohort of injection drug users in Baltimore, MD, 1988-2000[J]. Drug Alcohol Depend, 2006, 83(2): 147-156. DOI: 10.1016/j.drugalcdep.2005.11.007. -





 下载:
下载: