Study on relationship between hemoglobin content and blood pressure in pregnant women in Zhoushan islands
-
摘要:
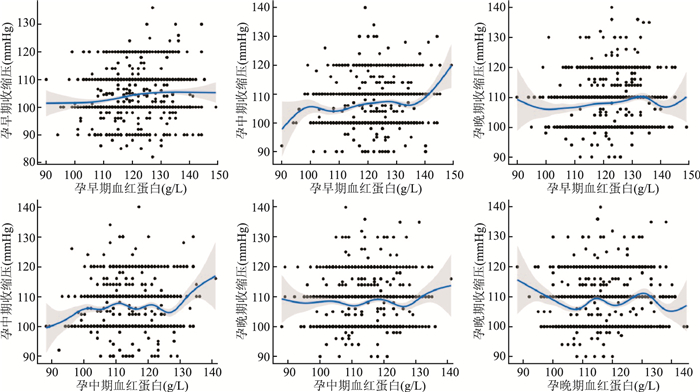
目的 探讨舟山地区孕妇妊娠期血红蛋白含量与血压的关系,为妊娠期高血压的病因学研究提供科学依据。 方法 采用回顾性调查研究,对2017年1月~2018年6月期间在浙江省舟山市妇幼保健院进行围产保健的1 383名孕妇孕早、中、晚期的血红蛋白含量与血压进行监测,采用多元线性回归分析不同孕期血红蛋白含量与血压之间的关系。 结果 孕早、中、晚期贫血发生率分别为7.74%、25.45%和15.76%;多元线性回归显示,孕期血红蛋白水平对孕早、中、晚期收缩压均有影响,并且呈现出越早期血红蛋白水平对各期的收缩压影响明显。早期的血红蛋白水平的影响最大(β=0.10,P < 0.001),中期无统计学关联,晚期的影响其次(β=0.04,P=0.027)。血红蛋白水平与舒张压水平的变化趋势类似于其与收缩压之间的关系。 结论 妊娠期血红蛋白水平对孕早、中、晚期血压均有明显的影响,定期测量孕期血红蛋白水平,可以更好地改善孕产妇健康状况。 Abstract:Objective To investigate the relationship between hemoglobin and blood pressure of pregnant women in Zhoushan islands, so as to provide scientific evidence for the etiological study of gestational hypertension. Methods A retrospective study was conducted among 1 383 pregnant women who received perinatal care in Zhoushan Maternal and Child Health Hospital of Zhejiang Province from January 2017 to June 2018. Pregnant women were monitored for hemoglobin content and blood pressure in the early, middle and late pregnancy. The multivariate linear regression was used to analyze the relationship between hemoglobin content and blood pressure in different pregnancy. Results The incidence of anemia in early, middle and late pregnancy was 7.74%, 25.45% and 15.76% respectively. The multivariate linear regression showed that hemoglobin levels during pregnancy had effects on systolic blood pressure in early, middle and late pregnancy, and the earlier hemoglobin levels were monitored, the more obvious the effect on systolic blood pressure was.With the increase of hemoglobin level, systolic blood pressure increased, such as the effect of hemoglobin on systolic blood pressure in early pregnancy, mid-pregnancy and late pregnancy. Hemoglobin of first trimster had the greatest effect (β=0.10, P < 0.001), Hemoglobin of second trimester had no obvious effect, and that of third trimester had the second effect (β=0.04, P=0.027).Hemoglobin levels and diastolic blood pressure levels were similar to their relationship with systolic blood pressure. Conclusions Hemoglobin levels during pregnancy have significant effects on systolic and diastolic blood pressure in first, second and third trimsters of pregnancy. Regular measurement of hemoglobin levels during pregnancy can improve the health of pregnant women. -
Key words:
- Pregnancy /
- Hemoglobin /
- Blood pressure
-
表 1 研究人群的基本特征(n=1 383)
Table 1. Basic characteristics of the study population (n=1 383)
变量 孕妇 年龄(岁) (x±s) 27.58±3.03 文化程度[n(%)] 初中以上 1 224(88.50) 初中及以下 159(11.50) 孕前BMI(kg/m2) [n(%)] < 18.5 314(22.70) 18.5~ 938(67.82) > 24.9 131(9.47) 分娩孕周(x±s) 39.03±1.08 子代性别[n(%)] 男 774(56.97) 女 609(44.03) 表 2 孕妇各孕期的基本特征(N=1 383)
Table 2. Basic characteristics of pregnant women in each pregnancy period (N= 1 383)
变量 孕早期 孕中期 孕晚期 各期贫血人数[n(%)] 107(7.74) 352(25.45) 218(15.76) 各期血红蛋白(g/L, x±s) 125.04±8.94 114.02±8.55 115.88±9.22 各期收缩压(mmHg, x±s) 104.20±8.04 106.39±7.37 108.04±9.05 各期舒张压(mmHg, x±s) 70.80±7.65 73.88±7.52 73.80±7.57 各期增重(kg, x±s) 0.83±1.74 7.67±2.43 4.55±1.68 表 3 孕期各期血红蛋白与收缩压的关系
Table 3. Association between hemoglobin and systolic blood pressure during different trimesters of pregnancy by multiple linear models
孕期 血红蛋白 β Sx P值 早期血红蛋白与早期收缩压a 孕早期 血红蛋白 0.13 0.02 0.001 早中期血红蛋白与中期收缩压b 孕早期 血红蛋白 0.11 0.02 < 0.001 孕中期 血红蛋白 -0.02 0.03 0.427 早中晚期血红蛋白与晚期收缩压c 孕早期 血红蛋白 0.10 0.03 < 0.001 孕中期 血红蛋白 -0.03 0.04 0.383 孕晚期 血红蛋白 0.04 0.03 0.272 注:a表示调整孕妇文化程度、年龄、孕前BMI、测量血压时的孕周、孕早期增重; b表示调整孕妇文化程度、年龄、孕前BMI、测量血压时的孕周、孕早期增重和中期增重; c表示调整孕妇文化程度、年龄、孕前BMI、测量血压时的孕周、孕早期增重、中期增重和晚期增重。 表 4 孕期各期血红蛋白与舒张压的关系
Table 4. Association between hemoglobin and diastolic blood pressure during different trimesters of pregnancy by multiple linear models
孕期 血红蛋白 β Sx P值 早期血红蛋白与早期舒张压a 孕早期 血红蛋白 0.15 0.03 < 0.001 早中期血红蛋白与中期舒张压b 孕早期 血红蛋白 -0.06 0.02 0.012 孕中期 血红蛋白 0.15 0.03 < 0.001 早中晚期血红蛋白与晚期舒张压c 孕早期 血红蛋白 -0.03 0.02 0.240 孕中期 血红蛋白 0.01 0.03 0.704 孕晚期 血红蛋白 0.09 0.03 0.001 注:a表示调整孕妇文化程度、年龄、孕前BMI、测量血压时的孕周、孕早期增重; b表示调整孕妇文化程度、年龄、孕前BMI、测量血压时的孕周、孕早期增重和中期增重; c表示调整孕妇文化程度、年龄、孕前BMI、测量血压时的孕周、孕早期增重、中期增重和晚期增重。 -
[1] Zhong Q, Xu JY, Long YQ, et al. Interaction of body mass index and hemoglobin concentration on blood pressure among pregnant women in Guangxi, China[J]. BMC Public Health, 2014, 14: 474. DOI: 10.1186/1471-2458-14-474. [2] 李玉艳, 武俊青, 赵瑞, 等. 母亲妊娠后期和围生理期因素与青少年血压的关系[J]. 中华疾病控制杂志, 2016, 20(1): 34-37, 41. DOI: 10.16462/j.cnki.zhjbkz.2016.01.009.Li YY, Wu JQ, Zhao R, et al. The relationship between maternal gestational and perinatal factors and blood pressure among adolescents[J]. Chin J Dis Control Prev, 2016, 20(1): 34-37, 41. DOI: 10.16462/j.cnki.zhjbkz.2016.01.009. [3] 王红菊, 魏兆莲, 王素芳, 等. 饮食和生活方式的咨询指导对孕妇体重指数及妊娠结局的影响[J]. 中华疾病控制杂志, 2014, 18(4): 301-303. http://zhjbkz.ahmu.edu.cn/article/id/JBKZ201404008Wang HJ, Wei ZL, Wang SF, et al. The influence of consulting diet and life style systematically on BMI and pregnancy outcomes in women[J]. Chin J Dis Control Prev, 2014, 18(4): 301-303. http://zhjbkz.ahmu.edu.cn/article/id/JBKZ201404008 [4] Jwa SC, Fujiwara T, Yamanobe Y, et al. Changes in maternal hemoglobin during pregnancy and birth outcomes[J]. BMC Pregnancy Childbirth, 2015, 15: 80. DOI: 10.1186/s12884-015-0516-1. [5] 钟海兰, 卢新政, 陈秀梅, 等. 外周血中血红蛋白含量与血压水平的关系[J]. 中华高血压杂志, 2008, 16(12): 1111-1114. DOI: 10.16439/j.cnki.1673-7245.2008.12.006.Zhong HL, Lu XZ, Chen XM, et al. Relation between hemoglobin and blood pressure[J]. Chin J Hypertension, 2008, 16(12): 1111-1114. DOI: 10.16439/j.cnki.1673-7245.2008.12.006. [6] 高宇. 孕晚期高浓度血红蛋白与妊娠不良结局的关系[J]. 海南医学, 2011, 22(11): 100-101. DOI: 10.3969/j.issn.1003-6350.2011.11.044.Gao Y. Association between high hemoglobin level of third trimester of pregnancy and adverse outcome[J]. Hainan Medical Journal, 2011, 22(11): 100-101. DOI: 10.3969/j.issn.1003-6350.2011.11.044. [7] 乐杰, 谢幸, 林仲秋, 等. 妇产科学-第7版[M]. 北京: 人民卫生出版社, 2008.Le J, Xie X, Lin ZQ, et al. Obstetrics and gynecology-seventh edition[M]. Beijing: People's Health Publishing House, 2008. [8] 蒲柳艳, 吴金华, 黄满仙, 等. 浙江省舟山市40819名孕妇妊娠期血压变化趋势及影响因素研究[J]. 疾病监测, 2018, 33(9): 770-774. DOI: 10.3784/j.issn.1003-9961.2018.09.016.Pu LY, Wu JH, Huang MX, et al. Study on change trend of blood pressure and related factors in 40819 pregnant women in Zhoushan, Zhejiang[J]. Disease Surveillance, 2018, 33(9): 770-774. DOI: 10.3784/j.issn.1003-9961.2018.09.016. [9] Huisman A, Aarnoudse JG. Increased 2nd trimester hemoglobin concentration in pregnancies later complicated by hypertension and growth retardation. Early evidence of a reduced plasma volume[J]. Acta Obstet Gynecol Scand, 1986, 65(6): 605-608. DOI: 10.3109/00016348609158396. [10] Heilmann L, Rath W, Pollow K. Hemorheological changes in women with severe preeclampsia[J]. Clin Hemorheol Microcirc, 2004, 31(1): 49-58. DOI: 10.1177/107602960401000116. [11] 姚立岩, 柏学民, 张毓洪, 等. 妊高征危险因素调查分析[J]. 中国妇幼保健, 2004, 19(10): 116-117. DOI: 10.3969/j.issn.1001-4411.2004.20.070.Yao LY, Bai XM, Zhang YH, et al. Investigation and analysis of the risk factors in women with pregnancy-induced hypertension syndrome[J]. Maternal and Child Health Care of China, 2004, 19(10): 116-117. DOI: 10.3969/j.issn.1001-4411.2004.20.070. [12] Cabrales P, Han G, Nacharaju P, et al. Reversal of hemoglobin-induced vasoconstriction with sustained release of nitric oxide[J]. Am J Physiol Heart Circ Physiol, 2011, 300(1): H49-H56. DOI: 10.1152/ajpheart.00665.2010. [13] Davis MR, Fitzpatrick CM, Dixon PM, et al. Thrombus-induced endothelial dysfunction: Hemoglobin and fibrin decrease nitric oxide bioactivity without altering eNOS[J]. J Surg Res, 2004, 122(1): 121-129. DOI: 10.1016/j.jss.2004.07.009. [14] Brannon PM, Taylor CL. Iron supplementation during pregnancy and infancy: uncertainties and implications for research and policy[J]. Nutrients, 2017, 9(12): 1327. DOI: 10.3390/nu9121327. -





 下载:
下载: